Did you know 92% of Americans would consider delaying dental care due to cost, and one in five skip it entirely? As financial pressures grow, demand and cost for braces are rising, but many households are putting off non-urgent dental treatments.
That’s why Risas Dental is stepping in to bridge that gap, making orthodontic care truly accessible for every patient, regardless of background.
To better understand how access and affordability are reshaping orthodontic demand, we analyzed data revealing who is getting braces, how they’re affording it, and why more adults in Arizona, Colorado, Texas, and Nevada are choosing treatment.
Who is getting braces in 2026?
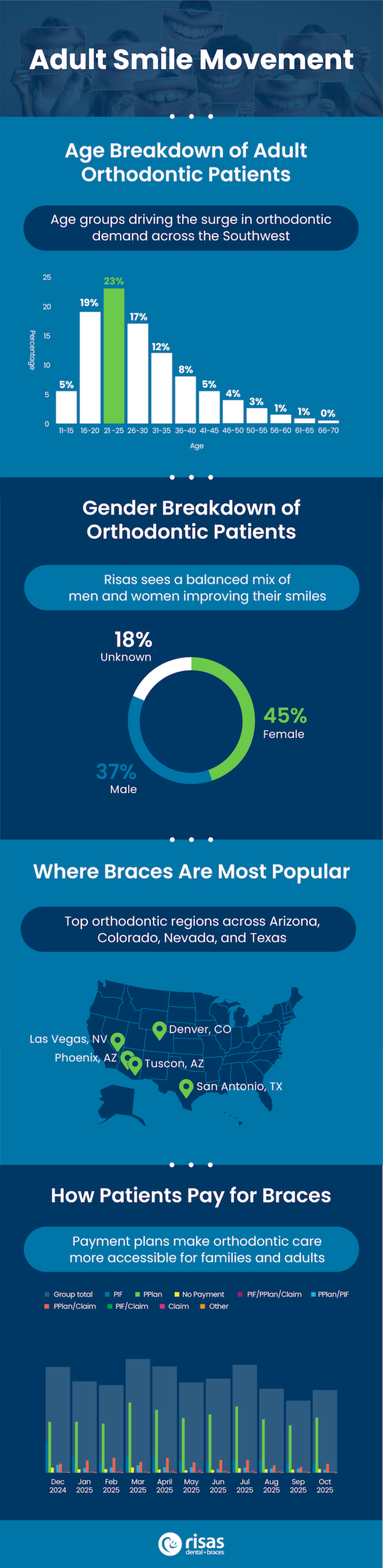
There is an upward trend among adults aged 25-45 choosing orthodontic treatment, driven by cost accessibility, a renewed focus on appearance, and functional dental benefits. Those aged 21-35 make up 50% of all orthodontic patients.
Our dental data found that women are slightly more likely than men to pursue orthodontic treatment, but the percentage difference is slim, suggesting that overall the audience is gender-balanced.
The top-performing regions for orthodontics are Phoenix, Denver, Tucson, Las Vegas, and San Antonio. Specifically, Aurora North saw the highest number of procedures compared to other cities, with well over 1,000. South Tucson saw 750, followed by Federal Heights.
So, if the demand for braces is rising, yet the percentage of Americans delaying or skipping dental care is huge, how are people affording it?
At Risas Dental, we offer several payment options to choose from, making dental care more affordable. Most of our patients select our payment plans to help spread the cost over weeks or months, making dental costs much more accessible for families and adults in 2026.
Risas dental care standards
There are many reasons someone may need braces, from improved oral health and reduced jaw pain to better confidence and self-image.
To highlight a few more reasons why people are prioritizing braces in 2026, we asked real patients how braces helped them.
Life-saving braces intervention
In El Mirage, we’ll never forget this incredible story of when a child needed an emergency dentist in Phoenix after a dangerous accident.
“My daughter had a serious scooter accident… her two front teeth suffered 50–75% avulsion, but her braces kept them in place. I contacted 20+ dental clinics, and no one would help. Risas Dental acted immediately and likely saved my daughter’s teeth. Their staff was exceptional, attentive, compassionate, and highly professional.”
Braces can be instrumental in urgent care needs and can have life-changing impacts on patients.
Same-day affordable braces
Risas strives towards being affordable and accessible to all families, so when Megan needed a dentist in South Tucson, she was in safe hands with us.
“Dr. Hooper and Dr. Hobson were great! They got my daughter’s braces on the same day as her cleaning. The team walked us through every step, and it was very affordable. Overall, a wonderful experience!”
Long-term transformation journey
Stephanie went to a dentist in Phoenix for braces, and the journey led her to renewed confidence and better dental health. She said,
“I was recommended to come here for my orthodontic journey, and I’m glad I did! I just got my braces off, and I’m happy with my results. Dr. Piekarsky was the best. He kept me informed throughout the whole process.”
Improving your oral health as an adult
We asked a Risas Dental spokesperson what they made of our findings.
“It’s never too late to improve your oral health. More adults are choosing braces now than ever before because they understand orthodontics goes beyond aesthetics. Straightening teeth and bite alignment can not only enhance confidence but also improve digestion, reduce jaw pain, improve speech, and protect against long-term issues like gum disease and tooth decay.
“At Risas Dental, we’re committed to making those benefits accessible to every patient. We offer two orthodontic options to meet different needs. Our easy-maintenance metal braces are a budget-friendly choice for the entire family, or we often recommend our ceramic braces for adults looking for a more subtle way to enhance their smile.”
Book a consultation with Risas today
If you’re ready to take the leap and improve your oral health, our team is here every step of the way. Risas Dental has trusted clinicians across the Southwest, making it simple to access the care you need, whether that’s orthodontics, routine dentistry, or urgent support
From finding an emergency dentist in San Antonio to visiting a dentist in Denver, or scheduling with an implant dentist in Las Vegas, our clinics are ready to give you affordable, patient-first care wherever you are.
When it comes to your smile, there’s no better time to start. Book your orthodontic consultation today.
All the above data was provided to C3 by Risas Dental and Braces' internal data team and is correct as of November 2025.
The state of children’s oral health
Many of the most common oral health issues begin at home, specifically with childhood habits. Poor routines developed early can lead to long-term dental issues, from cavities and gum disease to confidence issues and costly treatments.
So, how often are kids really brushing? Are trips to the dentist a regular occurrence? And how confident do parents feel about teaching their children the right oral hygiene techniques?
To find out, the team at Risas Dental conducted a survey of 1,500 parents to uncover the current state of children’s oral health. From brushing battles to sugar struggles, the results reveal what’s really going on when it comes to oral hygiene in American households.

Brushing battles & bathroom routines
When it comes to their children’s dental hygiene, most parents feel as though they have things under control. We found that 87% of parents are confident about family brushing habits, with just 9% expressing doubt. Confidence is the highest among parents with 1-2 children (86-88%), yet it dips to just 76% in families with four or more kids. This suggests that the more children in the home, the harder it might be for parents to keep tabs on everyone’s brushing routines.
Digging deeper, a quarter of parents admit that getting their kids to brush daily is a battle, with this struggle worsening in households with 3 or more children (where 37% often face resistance). Still, 28% of our participants revealed that their kids willingly brush on most days of the week.
However, despite good intentions, 51% of children are finding ways to dodge brushing altogether. Nearly half (47%) are only brushing for a few seconds, 13% are skipping toothpaste, and 25% are pretending to brush. These behaviors become more common as family size increases, rising from 21% in a one-child family to 32% in a 3-child family.
Parental role modeling influences the hygiene habits children adopt too. We found that 59% of kids see their parents brush twice a day. Meanwhile, 23% see them brush once a day, and a smaller but still notable percentage (3%) never see their parents brush at all. On average, children are brushing independently at 4.36 years old, and in big families, solo brushing starts as young as 2.7 years.
We also found a strong desire among parents for schools to step in, with 87% believing that dental hygiene (particularly effective brushing) should be taught in the classroom.

Snacks, sugar & shortcuts
Diet plays a crucial role in oral hygiene too, and it appears that many children are being exposed to significant amounts of sugar.
We found that commonly consumed items include flavored milk (59%), juice (57%), and fruit snacks (51%). Almost half of those we surveyed said that their children consume ice cream and fast food regularly, too.
What’s more, parents with more children are more likely to allow sugary treats and drinks, with this combination of sugar and short brushing times putting children at a higher risk of issues down the line.
Tooth Fairy economics
While it might just seem like a fun tradition, the Tooth Fairy can offer an interesting glimpse into how families value and engage with their children’s oral health.
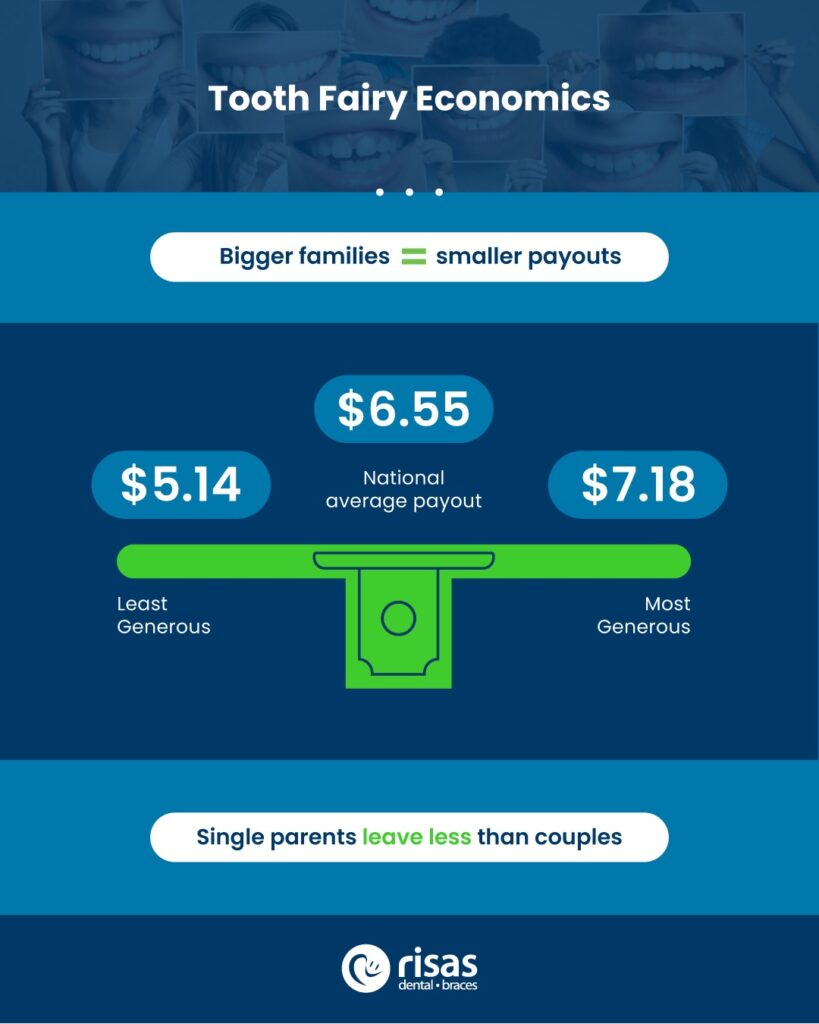
When asked about how much they typically leave under their kids’ pillow, the average stands at around $6.55, with 39% of parents leaving between $2–$5. Single parents tend to leave slightly less ($5.65), compared to couples ($7.02).
The most generous payouts come from two-child families (averaging $7.18 per tooth), while families with four or more kids leave an average of $5.14.
While the amount left doesn’t directly reflect brushing habits or tooth health, it does signal how families recognize dental milestones. A visit from the Tooth Fairy can be more than just exciting for kids, it can help build positive associations with taking care of their teeth.

Teeth, teasing & well-being
Dental hygiene is important for more reasons than one. Inadequate care can lead to teasing and future confidence issues in children, with kids becoming sensitive about their teeth.
Our survey revealed that 26% of children have been teased about their teeth before, with this rising to 33% in 2-child families. We also found that many children are missing activities due to dental issues, including school (16%), sports (11%), and family events (13%). Missing meals (17%) and sleep disruption (16%) were also brought up as additional issues.
As for how children feel about their teeth, 45% reported feeling confident and proud, while 32% feel more neutral about their smiles. A smaller group struggles with negative emotions, with 7% feeling anxious, 6% feeling embarrassed, and 5% feeling frustrated.
Interestingly, children in larger families (4+ children) are the most confident (57%), despite more shortcuts and diet drawbacks.
Final thoughts
So, what can we take away from our survey on the state of children’s oral health? Here are some final insights from our Risas Kids Clinical Director, Dr. Elizabeth Walton:
“The survey highlights the vital role parents play in shaping their children’s oral health, as well as the unique challenges they face, especially those with multiple children. Whether it’s modeling proper brushing, establishing consistent routines, or seeking expert advice, parents are the first line of defense against stopping dental issues before they arise.”
“Finding the time to supervise your children until they can confidently brush solo is key, as well as encouraging them to brush twice a day for at least two minutes. Limiting sugary snacks, booking regular dentist visits, and flossing once they’re old enough are also crucial. Together, these habits can help prevent costly problems.”
“Our findings make another thing clear: oral health impacts much more than just a child’s smile. With more than a quarter of kids admitting to being teased about their teeth, and many more missing important activities due to dental issues, proper care, both at home and in professional settings, is essential.”
Well, there you have it: our insights on the state of children’s oral health across America. With effective brushing habits, as well as encouragement from parents and caregivers, children’s oral hygiene can dramatically improve, reducing the risk of long-term issues and expensive treatments.
It’s not only at-home care that’s crucial though, with regular check-ups also playing a key part in ensuring a healthy smile. If your child is due a check-up soon, you can browse our kids dental services for expert, personalized oral health guidance.
And if you’re in the Phoenix area, we now offer children’s dentistry at our first Risas Kids Dental office! With flexible early morning and after-school appointment times, plus free exams for children under two, we offer professional dental care for the whole family.
For more information on available treatments, browse our full list of locations. Or if you’re looking for additional insights, read a couple more of our blog posts including: How to make the first Tooth Fairy visit magical, and when do kids start losing teeth?
Methodology
3Gem survey of 1,500 US parents aged 18+ with children aged 2–15.
[LM1]Insert commentary explaining the long-term implications of poor brushing habits formed early in life, including preventable cavities, enamel erosion, and costly interventions.
Flossing is an essential part of practicing good oral health. While brushing is crucial for cleaning the surfaces of the teeth, flossing is crucial for cleaning food debris from all the nooks and crannies in between. It is the only way to effectively remove plaque and bacteria trapped between your teeth and below the gum line.
If left alone, this plaque and bacteria can build up and cause tooth decay, gum disease, and other health problems. Flossing helps maintain your teeth's structure and strength and may allow you to avoid complex dental work like fillings and root canals. The health of your teeth and mouth also impact the health of the rest of your body.
What happens if I don’t floss?
Failing to floss leaves food particles stuck between your teeth and gums that eventually break down into acids and sugars. Those compounds mix with saliva and leave a sticky, hard-to-remove build-up called plaque in those spaces. Over time, plaque will erode tooth enamel, which can result in cavities.
Once plaque accumulates and hardens, it is now tartar. Tartar can cause the gums to swell and bleed, and it can also cause gum diseases like gingivitis and periodontitis. Gum disease causes multiple oral and dental health issues like bad breath and premature tooth loss.
Gum infections can also contribute or exacerbate to other diseases. For example, it can make diabetes more difficult to manage due to spikes in blood glucose levels. Furthermore, if the bacteria from your mouth enter your bloodstream through an infection or cut, it can cause inflammation and blockages in blood vessels the heart or lungs.
Caring for Your Teeth and Gums
The American Dental Association (ADA) recommends brushing twice a day and flossing at least once a day. Pairing these habits with an antimicrobial mouthwash can also help, especially for patients with a history of gum disease.
When it comes to choosing the right floss, it’s all about what works best for you. Waxed or unwaxed floss, flavored or unflavored, there is no difference. You may also prefer picks, or water flossers. The ADA also works with some dental supply companies to test products and those that pass earn the ADA’s seal of approval, which is displayed on the product packaging. The ADA offers a convenient online database featuring approved products.
Regular dental checkups and cleanings help maintain good oral hygiene and prevent potential dental problems from developing into more serious issues. A dentist can identify signs of tooth decay, gum disease, or other oral health problems that may require treatment. They can also provide personalized advice for more effective home dental care and product recommendations to keep your teeth and gums healthy.
Bottom Line
Flossing is a crucial step in a healthy oral hygiene routine. Neglecting to floss can cause bad breath and lead to the buildup of harmful bacteria in the mouth, which can cause cavities, gum disease, and more serious health problems.
Good dental habits with dental checkups and cleanings can help you save money in the long run by preventing costly dental procedures. It only takes a few minutes each day to floss, but the benefits are significant for your overall oral health.
Schedule an appointment today so we can help you keep your smile healthy.
Frequently Asked Question (FAQs):
Is it really that bad if I skip flossing once in a while?
While the ADA recommends flossing once a day, we know that life happens. Sometimes you run out of time getting ready, run out of floss, or just plain forget. Not flossing becomes a problem when "once in a while" turns into a week or 2 at a time.
What are the early signs of gum disease?
Early (or mild) gum disease is known as gingivitis. Symptoms of this condition include:
- Red and/or swelled gums
- Bleeding gums especially during or after brushing or flossing
- Sensitive gums or sensitive teeth at the gum line
Can gum disease be reversed if I start flossing regularly?
Gum disease in the early stages is usually reversible, but your teeth will likely need more care than what you can do at home. A professional dental cleaning paired with more diligent care at home should have your gums healthy and disease-free. However, if your gum disease has progressed into periodontitis, only a dentist can treat it.
When should children start flossing?
The ADA recommends kids should begin flossing once they have two teeth touching each other. Parents are advised to complete this step until the child reaches 10 to 11 years old to ensure proper technique and effectiveness.
Do you dread going to the dentist? You're not alone – it's estimated that 36% of people experience dental anxiety and 12% suffer from extreme dental fear.
While common, it's not something you have to live with. Avoiding the dentist can significantly impact your oral health, especially because small dental problems can grow into large ones if left untreated.
Regularly visiting the dentist isn't just crucial for your oral health; it can also impact your overall physical health. Poor oral hygiene can lead to other health concerns like heart disease, pregnancy complications, diabetes, kidney issues, and more.
Before you start working on your dental fear, it's also vital to identify how severe your dental anxiety is. Someone with normal dental nerves will need much less work than someone with severe dental phobia. If you suspect you have extreme dental anxiety, it may be worth contacting a mental health professional directly to learn how to deal with these feelings.
Strategies to Manage Dental Anxiety
While dental anxiety can be difficult, we recommend trying these coping strategies.
- Open Communication
First, share what exactly you’re afraid of with your dentist so they can help devise a plan. For example, if you're scared of pain, they can tell you what level of discomfort to expect during your appointment and may offer local anesthesia. If your fear is more centered around being unsure of what to expect, then your dentist can help relieve your anxiety by explaining what they're about to do before they do it.
- Relaxation Techniques
When you have dental anxiety, it’s common to be nervous before, after, and during the appointment. Consider learning some relaxation techniques, like deep breathing exercises to help calm your worries. You can also calm yourself before the appointment by journaling to work through your thoughts, or by using meditation.
- Bring Distractions
Distracting yourself may sound like an obvious option, but it can help reduce anxiety. Listen to music, an audiobook, or a podcast, wear virtual reality goggles, or ask the staff to turn on the television if there’s one in the room.
- Gradual Exposure Therapy
Another option to reduce anxiety is to desensitize yourself through exposure. Talk to your dentist and see if they’ll let you come in a few times before your appointment to get used to the office and the equipment.
- Consider Dental Sedation Options
If your dental anxiety is intense, relying on dental sedation might be best. Your dentist can offer you nitrous oxide or oral sedatives during dental visits for more relaxation. However, dental sedation is offered at the dentist's discretion, so it's important to ask about this before your appointment.
- Building Trust and Support
Overcoming your dental fear is possible with treatment and proper support. We recommend that you seek support in and out of the dental office by talking with friends, family, or support groups along with finding a provider that works with and for you. Find an understanding dentist specializing in treating anxious patients. An uncompassionate dentist can worsen dental anxiety by pushing patients to do things before they're ready.
Book With Our Compassionate Dentists
Our dentists and teammates are always willing to work with you to make you feel as comfortable as possible, regardless of your level of dental anxiety. Schedule an appointment or give us a call today to find out how we can put you at ease and get you the dental care you need.
Understanding Dental Anxiety
Some of the most common causes and triggers of dental fear are:
- A negative dental experience in the past
- Fear of the loud and intimidating dental tools
- Fear of the pain and discomfort
- A fear of needles
- Concerns about your oral health
- Fear of receiving bad news
- Feeling embarrassed about your dental health
- Worries around being scolded by the dentist
- Feeling a loss of control
Frequently Asked Questions
How can I find a dentist who specializes in treating patients with dental anxiety?
Some dentists advertise that they specialize in handling dental anxiety. However, the best way to know is to talk to the office directly. Before you book an appointment, call the dental clinic and ask them if they've dealt with anxious patients in the past. Ask them to walk you through how they help to reduce dental fear in patients. If the clinic's techniques sound like they would work for you, it's a potential fit.
Is dental sedation safe?
There is a risk with any type of sedation, however the risk associated with dental procedures is small.
What are the different types of sedation?
There are four levels of dental sedation. Usually, minimal sedation is used in dental care.
- Minimal sedation: You're fully awake but relaxed and don't feel pain.
- Moderate sedation: You're conscious but may slur your words and not remember parts of the appointment.
- Deep sedation: You're almost unconscious but can be awakened if needed.
- General anesthesia: You're entirely unconscious.
Can I bring a trusted person with me to dental appointments for support?
Bringing a friend or loved one to support you can be a great way of soothing dental anxiety. We recommend that you notify your dental office beforehand to so they aren’t surprised and confirm that your support person can stay with you.
How can I maintain good oral health if I avoid dental visits due to fear?
Unfortunately, nothing can replace visits to a dental professional. Your dentist needs to see you at least every 6 months to check for problems you may not be aware of and address issues before they magnify. The best way to maintain your oral health is to find a dentist that works with you and your fear to help you stay healthy while attending your regular check-ups.
Is dental insurance worth it? The real costs of skipping the dentist
It's easy to find excuses not to go to your dental check-ups, especially when you’re worried about how you’re going to pay the check. If that’s you, you’re not alone – the 2025 Dental Report found that around 1 in 3 American adults have avoided a dental appointment in the last year, an unfortunate trend consistent with the findings over the past decade.
But with so many demands on our money every month, is dental insurance actually worth it? At Risas Dental and Braces, we’ve been investigating how much the average American adult is spending on dental care and what you risk spending on treatment in the long term when you skip routine visits.
Do I really need dental insurance?
The Dental Report found that, across the US, an estimated 34.1% of adults had skipped dental visits over the past year. That means one in three Americans didn’t see a dentist for routine check-ups - and the number one reason given for missing appointments is the prohibitive costs due to lack of access to dental insurance.
We get it; dental insurance can be expensive, and if you’ve never had any major issues with your teeth, it might feel like you can do without it, especially if your finances are stretched thin. But the longer you leave an untreated cavity or annoying toothache, the higher your chances of needing a root canal, crown or full tooth extraction, which means greater risk of dental complications and a much steeper bill to pay to get it fixed.
If you’re not sure whether dental insurance is worth it for you, consider if you could afford to look after your oral health if something did go wrong.
Highest cost increase for delayed treatment by state
At Risas Dental and Braces, we’ve carried out our own investigative research into how much the average American adult who regularly visits the dentist spends on dental care, versus how much they might spend if they skip the routine visits and avoid preventative dental care, to see if dental insurance is worth it.
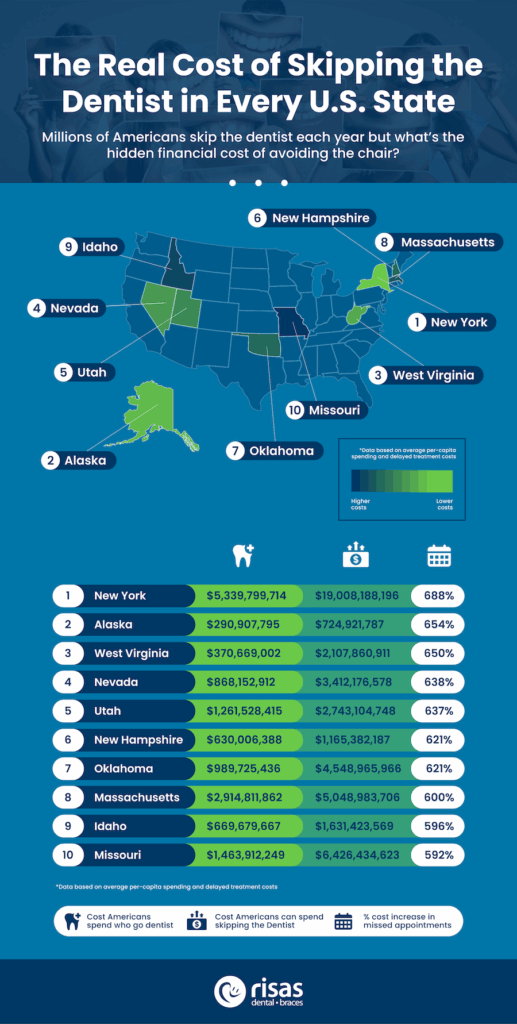
For each state, we looked at the:
- Annual dental spend of the average American adult who visits the dentist regularly
- Potential annual cost to treat oral health issues that often arise from lack of preventative care
- Percentage increase in overall costs for those who don’t visit the dentist regularly
Based on our research, we’ve identified the top five states where, if you don’t visit the dentist regularly, you’ll be shelling out the biggest increase in costs.
- Utah
Coming in at number five, the average spend on services for those regularly attending the dentist in Utah is $360 per capita. But when minor issues aren’t caught early, the cost of the delayed treatments comes out at $2,728 – this means that without preventative care, your costs could increase by 637%.
- Nevada
Next on the list is Nevada, with the average adult spending $361, compared with delayed treatment costs of $2,664, increasing your costs by 638%. Don’t forget, if you’re based in Nevada and looking for a compassionate, expert Las Vegas dentist with flexible payment options available to help you manage your finances, you can find two of our locations in North Las Vegas and Boulder Crossings.
- West Virginia
Those in West Virgina are paying the third-highest rates in the country for delayed dental treatments, averaging out at $2,744. While Wisconsin and Wyoming may both have higher costs associated with delayed treatment, individual patients in West Virginia can access much cheaper regular dental treatments at just $366, putting the increase in spend at an eye-watering 650%.
- Alaska
Alaska comes in with the one of the cheapest per capita spends on regular dental care in the country at just $340. So, while the cost of delayed treatment is similarly low - $2,564 – the percentage increase is stark at 654%.
- New York
With a low per-capita spend of $340, the cost of delayed treatment in New York averages out at $2,680, meaning those living in New York state who don’t visit the dentist for check-ups and critical preventative care risk spending an eye-watering 688% more on their dental health than those who do. Across the state, that comes in at over $19 million spent on delayed treatments per year!
Should I get dental insurance?
We spoke to Dr. Collin Bowerman to see what they made of our findings.
“Preventative dental care is the number one way to reduce your dental costs in the long run. Think about this – a minor problem, like filling a cavity, might cost you $100 to get fixed. If you ignore it, it won’t go away, and suddenly you could be facing treatments costing $1,000 or more.
“For those with access to it, we would highly recommend investing in dental insurance or a dental savings plan, so you can sidestep major health concerns and protect both your finances and your long-term health. Dental insurance typically covers those routine visits to the dentist, so all you have to do is show up. If you’re not able to invest in dental insurance, many practices – including here at Risas Dental and Braces – offer a variety of payment plans and affordable options to help alleviate your dental care costs.
“We appreciate that many families across America, for various reasons, can’t access dental insurance. Whatever your financial situation, the best thing you can do for your oral health is to come to the dentist as often as possible.”
To learn more about the different options available to you with Risas Dental and Braces – including 20% off treatments paid in full, a healthcare credit card or a personalized payment plan – please take a look at our payment options. We also offer memberships for individuals, two people or families of up to eight, providing a low-cost alternative to insurance regardless of your income or credit score.
Top tips to keep your dental spending down
Our experts have put together some ideas for how you can look after your own dental health and access any support that might be available to you.
- Stick to a good daily routine by brushing twice daily and flossing. This helps remove plaque, prevent cavities, and keep your gums healthy. Consistency is key to long-term oral health.
- Keep up with regular check-ups. Visit your dentist at least twice a year for cleanings and exams, even if you’re not experiencing any issues. Regular visits help catch potential problems early and keep your smile in top shape.
- Choose preventive treatments to protect your teeth and reduce the need for more complex treatment down the line.
Remember, no matter how long it’s been since your last visit to the dentist or what shape your teeth are in, our expert team is on-hand to provide personalized oral health care and guidance for you and your family. If you’ve not been to the dentist in a while, we have a video on what to expect and other helpful information on our blog.
Book an appointment now or search our locations with your zip code to see if we have a clinic near you.